
Diabetic Eye Care — Wisconsin's Trusted Eye Care Specialists
Diabetes Can Steal Your Sight —
Often Before You Notice Anything Is Wrong
If you've been diagnosed with diabetes, your eyes are at risk right now, even if your vision feels perfectly fine. Diabetic retinopathy, the leading cause of blindness in Americans under 65, often has no early symptoms. The only way to catch it is with a comprehensive diabetic eye exam. At Eye Care Specialists, we've been protecting Wisconsin families' vision for over 41 years, and we're here to help protect yours.
What is Diabetic Retinopathy?
Diabetic retinopathy is a serious eye condition caused by high blood sugar damaging the blood vessels in your retina. Those vessels can leak fluid, swell, or grow abnormally — blurring your vision and, without treatment, leading to permanent vision loss. Of the more than 30 million Americans with diabetes, up to 45 percent have some degree of retinopathy. It is the leading cause of blindness in Americans under age 65.
Types of Diabetic Retinopathy
Non-Proliferative (NPDR) — The most common form, accounting for 80 to 90 percent of cases. Small blood vessels in the retina become damaged and may leak fluid or blood. Many patients have no noticeable symptoms early on, which is why regular exams are critical. Without monitoring, 5 to 20 percent of NPDR patients may lose significant vision within five years.
Proliferative (PDR) — The more advanced and severe stage. The retina stops receiving enough oxygen and begins growing new, fragile blood vessels that can bleed, cause scar tissue, and lead to retinal detachment or glaucoma. PDR often has no early warning signs at all — making annual exams even more essential for long-term diabetics.

Blood sugar-related changes cause
the retinal blood vessels to leak.
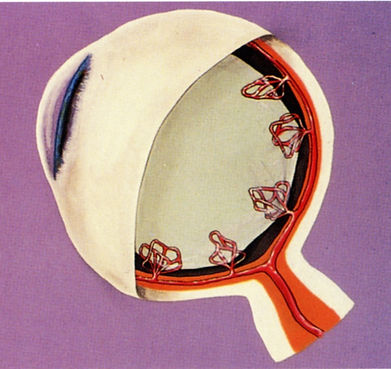
Blood sugar-related changes cause
new abnormal retinal blood vessels to grow.
Are You at Risk?
All people with Type 1 or Type 2 diabetes are at risk. These factors increase that risk further:
-
The longer you've had diabetes
-
Poor blood sugar control
-
High blood pressure
-
High cholesterol
-
Smoking
-
Being overweight
Managing these factors — combined with regular dilated eye exams — is your best defense against vision loss.
How We Detect and Monitor Diabetic Eye Disease
We use three advanced tools to catch diabetic retinopathy early and track changes over time:
-
Ophthalmoscopy — A detailed examination of your retina that identifies early signs like microaneurysms — tiny bulges in blood vessels that may leak fluid or blood.
-
Optical Coherence Tomography (OCT) — A fast, painless, noninvasive scan that creates detailed cross-sectional images of your retina. Similar to a CT scan, OCT measures swelling with exceptional accuracy and helps guide treatment decisions — often before you notice any vision changes.
-
Ultrasonic Testing — If bleeding makes it difficult to see the retina directly, ultrasound imaging helps us determine whether scar tissue or retinal detachment is present.
Treatment Options
Treatment depends on the type and severity of your condition. Our doctors will recommend the most appropriate approach for you.
Injection Therapy — Anti-VEGF medications (including Avastin, Eylea, Lucentis, and Vabysmo) are injected directly into the eye to reduce swelling and slow abnormal blood vessel growth. The procedure is quick and performed in our office with numbing drops. Many patients experience vision stabilization and in some cases improvement.
Laser Treatment — Laser photocoagulation seals leaking blood vessels and prevents the growth of new abnormal vessels. Performed in our office or outpatient surgery center, the goal is to stabilize the disease and protect your remaining vision.
Surgical Treatment — In advanced cases, a vitrectomy may be necessary to remove blood and scar tissue from inside the eye. This is recommended when complications like persistent bleeding or retinal detachment occur.
Don't Wait for Symptoms.
Diabetic retinopathy can progress silently — by the time you notice something is wrong, significant damage may already be done. At Eye Care Specialists, our doctors have been detecting and treating diabetic eye disease in Wisconsin for over 41 years. Early detection is the single most important step you can take to protect your vision.
Schedule your diabetic eye exam at one of our three convenient Milwaukee-area locations today.


